Above: Photo by Carolyn Lagattuta
As the world continues to grapple with the COVID-19 pandemic, UC Santa Cruz faculty are deploying their resources and expertise to help humanity find its way out of the grip of the deadly infection.
Faculty members are working on myriad COVID-related projects, including developing quicker tests for the virus, fine-tuning mathematical models that predict how the virus will spread, and developing remote patient-monitoring systems.
Here are a few of the projects UC Santa Cruz science and engineering faculty are working on.
Rebecca DuBois: Antibody evidence
Rebecca DuBois, an associate professor of biomolecular engineering with expertise in virology and vaccine development, is working on a serological test to identify people with previous exposure to COVID-19.
DuBois’s test determines the level of antibodies (proteins that fight the virus) in people’s blood, which shows if they were exposed. Her test produces results in 20 minutes, far shorter than the six hours it takes with the gold-standard test commonly used, Enzyme-Linked Immunosorbent Assay (ELISA).
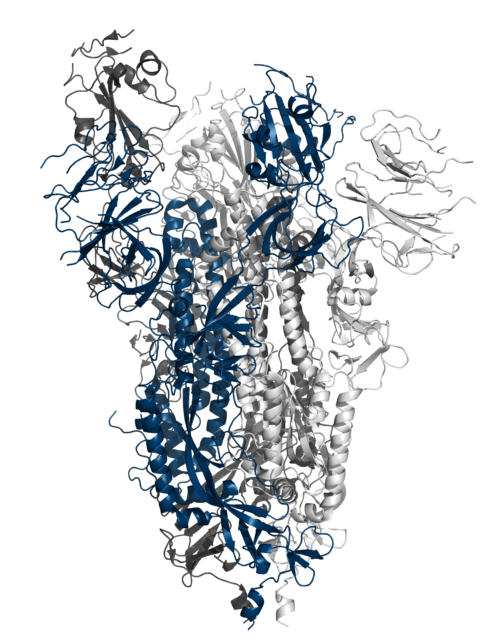
A molecular view of the coronavirus (SARS-CoV-2) spike antigen, courtesy Rebecca DuBois.
Her test is more sensitive than those currently available and will give the value of antibodies for each blood sample. Preliminary studies from her lab and other scientists are finding that antibody responses vary widely. As an example, one person may have antibodies 50 times less concentrated than another person, DuBois explained. It appears that people who have milder cases of COVID-19 have fewer antibodies.

Rebecca DuBois, associate professor of biomolecular engineering —Photo by Carolyn Lagattuta
The goal of DuBois’s new form of testing is to identify people who have lower risk of becoming infected and ill by determining the antibodies in their blood. Those people could be recruited for higher-risk activities like caring for patients with the virus and interacting with the public at stores.
She clarified that scientists don’t yet know what level of antibodies will provide protection—it could be that anyone with antibodies is protected or it could be that a certain threshold is required.
It’s still unknown how the antibody testing will be put to use, DuBois said, explaining that a lot will depend on funding for such studies. But the promise is compelling.
“We’re excited to bring a new technology to this field,” DuBois said.
Holger Schmidt: Chip potential
Holger Schmidt, professor of electrical and computer engineering, is also working on a method of faster testing. In his case, he and his colleagues are using optofluidic chip technology to detect RNA and antigen molecules and assess if an infection is present and how strong it is.

He uses small silicon chips to guide light to fluoresce tagged molecules. Using this method, health-care providers can get diagnoses quickly on-site, rather than waiting for samples to be sent away for test results. This method is also much more sensitive than the ELISA protein tests, Schmidt said.
In tests in the lab, the method allows scientists to see individual molecules in cell-isolate samples provided by the Centers for Disease Control.
“We’re testing that the principle really works, and it does,” Schmidt said, adding that the next step will be to run the test with nasal swab samples.
It will be at least a year, however, before the method can be used in a diagnostic setting. To make that happen, a lot of chips are needed and they need to run in the same way consistently. His plan is to involve a start-up he co-founded called Fluxus to commercialize the project.
Schmidt said it is exciting to work on something that has such an important use.
“I feel most excited for my graduate students,” he said. “It’s a really wonderful experience for them to see how lab research on a silicon chip can really be tied to what is on many people’s minds.”
Nader Pourmand: Nanosensor hopes
Nader Pourmand, a professor of biomolecular engineering, is testing a nanosensor technology that could provide quick, cheap serology tests that people could do daily at home to detect the level of antibodies to COVID-19.

Professor of biomolecular engineering, Nader Pourmand —Photo by Carolyn Lagattuta
The technology originated from nanopipettes that would evaluate a finger-prick blood sample, using disposable cartridges and a $100 reader that could be available at health clinics or pharmacies.
The cartridges would use nanosensor chips designed by Pinpoint Science, a company Pourmand cofounded.
The technology could be helpful in determining who gets a vaccine when one is developed. The tests would determine who has had COVID-19 and has immunity and then presumably might not need a vaccine, Pourmand said.
The technology could also allow people to easily test themselves every day.
“If I want to go to work, I can pay a couple of dollars to test myself and see if I am infected today or not,” Pourmand said.
But Pourmand faces significant hurdles before the technology can be used. Chip manufacturing is a big challenge as there is a backlog. Right now, he and his colleagues only have a few chips for testing. Once more are available, they will proceed to the next step to test on patients.
“My colleagues are literally working day and night to make it happen,” he said. “If we can make it, that would be a huge contribution.”
The UC Santa Cruz Molecular Diagnostic Lab: Quickly pivoting to meet the need

A UC Santa Cruz performing a COVID-19 test on themselves at one of the testing kiosks on campus. —Video still by Nick Gonzales
As a university without a medical school, UC Santa Cruz wasn’t the obvious choice to quickly set up a COVID-19 diagnostic lab. But that was what the campus was able to do thanks to fast action by three faculty members.
Olena Vaske, assistant professor of molecular, cell, and developmental biology; Michael Stone, professor of chemistry and biochemistry; and Jeremy Sanford, professor of molecular, cell, and developmental biology, worked together to build the lab from the ground up. It was a major endeavor as they had to comply with health privacy laws and numerous other regulations, said John MacMillan, associate vice chancellor for research.
“Bold leadership and bold decision making make a huge difference, and that’s what we’ve had on this campus,” he said. “Decisions had to be made very quickly.”
It helped a lot that Vaske had the credentials to run a diagnostic lab coupled with world-class expertise in RNA biology, MacMillan said.
The lab, which began operating in May, evaluates swabs for virus particles. It has tested students, staff, faculty, and community members referred from Santa Cruz Community Health and Salud Para La Gente (Health for the People). This past summer, the lab was on the way to handling 600–1,000 tests per day.
MacMillan said he is proud of the lab’s achievements.
“As researchers, we want to find a place to make a difference,” he said. “This has been an incredible opportunity to find a niche to make that happen.”
Narges Norouzi: Developing tools to manage from afar
Narges Norouzi, a teaching professor of computer science and engineering, is developing a video-assisted clinical care mobile device application that could help medical providers remotely manage patients with COVID-19.
The idea is that the app would collect clinically relevant information from the patient during a videoconference call with a physician. The app would record such info as blood oxygen saturation level, respiratory rate, and heart rate all in real-time.
Norouzi explained that the app would be able to get that info by interpreting the color changes in the patient’s face or fingertip. The information the app could pick up would be more sensitive than what a person could see themselves.
Norouzi is working with UC Davis Health Center to record data collected from COVID-19 patients. That data could be used to determine what factors correlate with hospitalization or people getting better or worse.
This past summer, Norouzi was preparing to start testing the system. She is happy that her work can potentially be useful to medical providers in their fight against COVID-19.
“The more tools we have at our disposal, the more prepared we are for the second or third wave,” she said.
Ricardo Sanfelice: Predicting the spread

Ricardo Sanfelice directs the Cyber-physical Systems Research Center and the Hybrid Systems Lab at UC Santa Cruz. —Photo by Carolyn Lagattuta
Ricardo Sanfelice, a professor of electrical and computer engineering, is working on developing mathematical models to predict the spread of COVID-19 around the world in different conditions.
He and his colleagues hope to come up with multiple models that describe what could happen with the coronavirus under different conditions. Policymakers could switch between the models as needed when deciding what actions to take.
Sanfelice is well aware that models have gotten a bad reputation with some for offering inaccurate predictions during the pandemic.
“All models are wrong, but some are useful,” he said. “What models can tell you is that if all these things happen as I expect, this is the potential outcome.”
He is collecting as much data as he can about what has already happened. His team is looking at the effect of different types of government actions on the virus spread, comparing the effects of the low-restrictions approach of Sweden to the more highly restrictive actions of New York and California.
“Looking at the past is easy,” he said. “Once you evaluate the past, you have confidence about the future.”
The development of the most useful mathematical models will take lots of work and high-performance computing power, but Sanfelice hopes the effort will contribute to society and humanity.
“This effort on COVID modeling has a direct impact right now,” he said.

